- med_admin
- 0 Comments
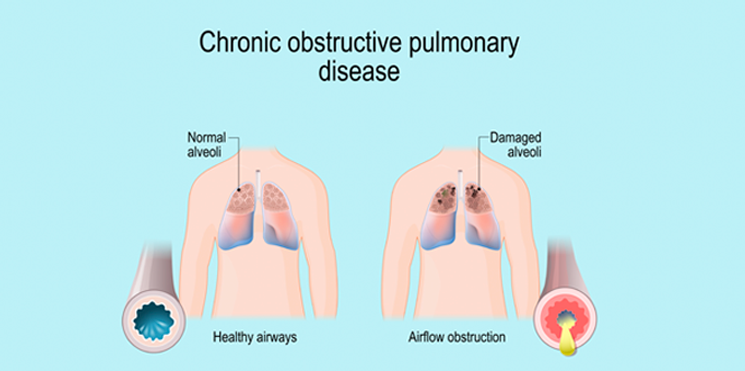
Chronic Obstructive Pulmonary Disease (COPD) and Emphysema
COPD is a term used for a class of diseases that cause slowly progressive lung damage. The term” chronic’ refers to the long term nature of the effects of COPD and ‘obstructive’ refers to the narrowing of airways causing difficult in breathing, chest tightness or wheezing. The disease is characterized by relatively irreversible changes in the airways (bronchioles or bronchi) as well as air sacs (or alveoli). Over time; there are changes in the blood vessels in the lungs as well.
Chronic bronchitis and Emphysema are the 2 commonly described types of COPD.
In emphysema, the predominant feature is destruction of the thin air sacs which leads to reduced oxygen exchange and in chronic bronchitis the predominant feature is narrowing of the airways with thickened lining and increased mucus production. Patients can have a combination of both features.
What are the symptoms of COPD?
Breathing difficulty, asthma-like symptoms like wheezing, chest tightness, decreased stamina, shortness of breathe on climbing stairs/walking up slopes/walking.
Persistent cough, with phlegm production for most of the year. The phlegm is usually white/cream/beige.


What causes asthma?
Family History-While no single culprit gene has yet been identified, asthma has been seen to run in families.
Early exposure in childhood to certain infections or toxins can make the lungs and airways more susceptible to asthma later in life.
Immune system – The immune systems response to certain triggering factors like dust, smoke, pollen, hair (fur/ dander) from animals, preservatives, emotional stress. stomach acid from acid reflux disease, and certain medications can cause the changes in the airways which lead to the development of asthma.
Asthma does not affect everyone in the same way.
Typically, patients with emphysema have shortness of breath as their predominant complaint and those with chronic bronchitis have chronic cough with sputum. However, patients can have a combination of both. In cases of worsening COPD, or a COPD attack, symptoms which should prompt an immediate evaluation by your doctor are:
- A change in the quantity, thickness, or colour of the sputum (yellow, green, brown) or the presence of blood streaks in the sputum
- Increasing shortness of breath or wheezing even with normal activity
- Fever, Sleep disturbance due to breathing difficulty more than once/night, more than once/week
- Leg swelling which persists even after sleeping with feet raised up on a pillow
- Confusion, increasing sleepiness is a warning sign of increasing carbon dioxide levels which can be dangerous
Patients are advised
- NOT to self medicate with extra doses of deriphylline like medicines (as they can have significant side effects)
- NOT to increase their oxygen Liter flow (if they are on home oxygen) without consulting their doctor.
- NOT to smoke, especially if they are using home oxygen due to the potential for causing a fire hazard
- NOT to take codeine or cough suppressants without their doctor's advice
Watch Latest Our Work
Frequently Asked Questions
Prevalence of COPD, Approximately 15 million people in India have Chronic Bronchitis based on projected estimates from 2011 census. In USA, COPD is the fourth leading cause of death. COPD is a significant global health problem.
The majority of COPD cases are caused by exposure to tobacco smoke.
In people who are not smokers, COPD can be caused by exposure to other types of smoke such as wood-smoke, coal (Bio-mass fuel exposure). This type of COPD is seen in women who cook on stoves with biomass fuels in poorly ventilated homes.
In a very small percentage of patients it is caused by a genetic deficiency in an enzyme called Alpha-1 antitrypsin. By and large, tobacco smoke is the culprit in almost all COPD cases.
Your doctor will request some tests after a detailed history and clinical examination.
Breathing tests Lung function tests -Spirometry, lung volume measurement and diffusion capacity for carbon monoxide (DLCO) are some of the tests your doctor may request.
Blood Tests – Arterial blood gas is a special blood test done where blood is drawn with a very fine needle from a blood vessel at the wrist. This gives information about oxygen content as well as carbon dioxide levels in the blood. It gives valuable information about the lung function in terms of how well the lungs are able to get rid of carbon dioxide and extract oxygen from the air inhaled.
Imaging – Your doctor will request for a Chest X-ray Sometimes a CT scan of the chest may also be necessary.
Exercise Oximetry – A measurement of oxygen saturation at rest and after exercise can give your doctor information about your oxygen requirements.
Sputum Culture
Bronchoscopy – Some patients may require an endoscopic examination of the airways.
It is important to understand that most of the changes in the lungs in COPD are irreversible. Thus the goal of treatment is to prevent further damage and preserve optimal lung function for as long as we can.
The most important part of treatment in COPD is helping Smokers to quit.
There are various medications and supportive therapies available to help patients who smoke drop the habit.
Stopping smoking is the MOST important aspect of treatment of COPD as it prevents further damage to already damaged lungs. Our center offers extensive assistance to patients who want to quit smoking.
Medications: Various inhaled medications are available for decreasing the symptoms. These are bronchodilators help to relieve the narrowing of the airways. Inhaled anti-inflammatory medications are also used. They are available in various forms such as Rotacaps with Rotahalers, Metered Dose inhalers, Diskus inhalers and Nebulisers.
Your doctor will sometimes prescribe combination of medicines to achieve better relief of symptoms. In addition at times of attacks or worsening symptoms, patients may need oral anti-inflammatory medications (a short course of steroids may be necessary), antibiotics maybe needed.
Theophylline:Some patients with longstanding COPD may need theophylline derivatives. However, your doctor will assess the need for this and prescribe accordingly. It is important not to exceed the dose prescribed or self medicate with this medication as they have serious side effects in higher doses and also cross interact with antibiotics.
Oxygen: Some patients with longstanding COPD may require short or long term oxygen therapy at home.
BIPAP: Some patients with longstanding sever COPD who have high carbon dioxide levels will need a special mask which blows air under pressure to assist their breathing at night.
Procedures/Surgery: Certain special types of emphysema cases can benefit from Lung Volume reduction procedures. This can be done via specialised Interventional Bronchoscopic procedures using special equipment – thermal vepor ablation. It can also be done surgically.
- Give up Smoking – This is the single most important lifestyle commitment.
- Avoid Infections – Infections in patients with COPD take a toll on their already weakened lung health. While it is not always possible to prevent infection, there are ways to minimise the chances of falling seriously ill. Get annual vaccination to prevent the flu. Wash hands with soap and water frequently. Keep inhalers and nebulizer equipment clean.
- Breathing methods – Pursed lip breathing exercises. Your health care provider will teach you breathing techniques which are very helpful in relieving symptoms.
- Techniques to bring up phlegm patients with chronic bronchitis benefit from learning techniques like deep coughing, huff coughing. There are also some devices available which help to loosen up the phlegm and cough it out. Some medications also help in making the mucus thinner and easier to cough out.
- Nutrition A well balanced nutritious diet is important to maintain good health and boost immunity. Ensure adequate protein intake and also vegetables and fruits. If you are underweight, the diet must be focused on increasing protein intake and achieving optimal weight. If overweight, the diet plan must be to lose weight. Obesity has more significant implications for people with higher carbon dioxide levels as well.
- Exercise Walking, stationary cycling are good exercises. In addition some exercises help patients with COPD to use their chest wall and stomach muscles better to assist their breathing. Such as shoulder squeeze, Shoulder horizontal abduction, modified knee bends. The physical therapists at our center can help patients to learn and practise these exercises. The breathing techniques mentioned earlier help patients with COPD overcome the feeling of difficulty breathing while exercising.
- Environment – Reducing air pollution- indoor and outdoor.
- Travel It is important to consult your doctor regarding air travel or travel to mountainous regions if you have moderately severe or severe COPD. Your doctor will assess the need for oxygen on aeroplanes or at high altitude.
- Travel It is important to consult your doctor regarding air travel or travel to mountainous regions if you have moderately severe or severe COPD. Your doctor will assess the need for oxygen on aeroplanes or at high altitude.
- Equipment Make sure that your nebulizer equipment, face mask and assisted cough devices like acapella/lung flute are kept clean to prevent infections.
- Collaborative Effort – Leading an active life with COPD will require a collaborative effort by the patient, the family and the health care personnel. Our goal is to offer you all the information to help you understand and take control of your health.